Spinal stenosis causes real, limiting pain – but surgery isn’t your only option. For many people in Lancaster dealing with this condition, gentle, nervous system-focused care can reduce pain, improve mobility, and help the body adapt in ways that make daily life manageable again. The key is understanding what’s actually happening in your spine, and what your options really are.
What Is Spinal Stenosis?
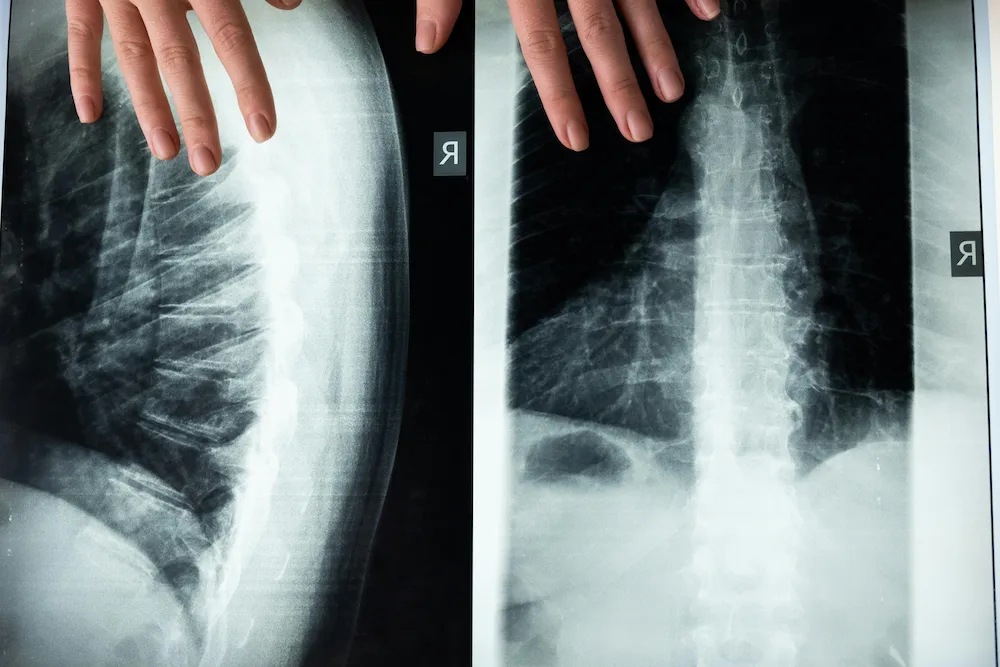
Spinal stenosis is a narrowing of the spinal canal – the channel that runs through your vertebrae and houses your spinal cord and nerve roots. When that canal narrows, it puts pressure on the nerves inside. That pressure is what causes the pain, numbness, and weakness that people with stenosis experience.
It most commonly develops in the lower back (lumbar stenosis) or the neck (cervical stenosis), though it can occur anywhere along the spine. For most people, it develops gradually over years, usually as a result of age-related changes like bone spurs, thickened ligaments, or disc degeneration.
The symptoms can vary quite a bit depending on where the narrowing is and how severe it’s become. Some people notice it most when walking or standing for extended periods. Others feel it as a constant ache, or as tingling and numbness that travels into the legs or arms.
Common Spinal Stenosis Symptoms
If you’re dealing with spinal stenosis, you’ve probably recognized at least a few of these:
Leg pain or cramping when walking. This is one of the most classic signs of lumbar stenosis. Many people find that they can only walk a short distance before the pain forces them to stop and rest – and that sitting or leaning forward brings relief. This pattern is called neurogenic claudication.
Numbness or tingling in the legs or feet. Compressed nerves don’t just cause pain – they also cause altered sensations. If you feel pins and needles, burning, or patches of numbness in your lower extremities, nerve compression is likely involved.
Balance problems. When the nerves responsible for sensing your body’s position in space are compressed, your balance and coordination can suffer. This is one of the more frustrating aspects of stenosis because it limits activity and increases fall risk.
Weakness in the legs. Some people notice that their legs feel heavy, fatigued, or difficult to control – especially after walking or standing. This is the nervous system struggling to communicate properly with the muscles.
Pain that improves with sitting or leaning forward. Flexing the spine slightly opens up the spinal canal, which temporarily relieves pressure on the nerves. This is why many stenosis patients instinctively hunch over a shopping cart or find that cycling is more comfortable than walking.
The Conventional Treatment Path – and Its Limitations
When most people get a spinal stenosis diagnosis, they’re typically offered a fairly predictable set of options: anti-inflammatory medications, physical therapy, steroid injections, and if those don’t work, surgery.
For some people, surgery is the right call – particularly when stenosis is severe and causing significant neurological deficits. But for many patients, the journey to surgery involves years of trying options that provide only temporary relief, followed by a procedure that carries real risks and a long recovery.
What often gets left out of that conversation is how much the nervous system itself contributes to the experience of spinal stenosis – and what can be done to work with it, rather than just addressing the structural narrowing.
The Nervous System’s Role in Spinal Stenosis Pain
Here’s something most people aren’t told: two patients can have the exact same degree of structural narrowing on an MRI and experience completely different levels of pain. One person might be debilitated; the other might have minimal symptoms.
The difference often comes down to how their nervous system is processing and responding to the compression. When the nervous system is already under stress – already running in a defensive, fight-or-flight state – it amplifies pain signals. Everything feels worse. Recovery is slower. The body doesn’t adapt.
This is why treating the nervous system directly, not just the structural issue, can make such a meaningful difference for people with spinal stenosis.
How Network Spinal Care Approaches Spinal Stenosis
Network spinal care is a gentle, nervous system-focused approach that uses light, specific touches along the spine – not forceful adjustments or cracking. The goal isn’t to force the canal to widen. That’s not possible with any conservative care. The goal is to help the nervous system shift out of defense mode so the body can use its own resources more effectively.
When the nervous system is less stressed, muscles around the spine tend to relax. Postural patterns shift. The body finds new ways to move that reduce the load on compressed areas. Inflammation – which is heavily regulated by the nervous system – often decreases. And the pain experience, which is always filtered through the nervous system, becomes less amplified.
In my practice, I’ve worked with patients in Lancaster who were told surgery was their only real option. Some of them had been living with stenosis for years, had tried injections and physical therapy, and were skeptical that anything gentle could help. For a significant number of them, network spinal care reduced their pain and improved their quality of life in ways they hadn’t expected.
That said, I want to be clear: network spinal care isn’t a cure for spinal stenosis. The structural narrowing doesn’t disappear. What changes is how the body relates to that narrowing – and for many people, that change is enough to make daily life functional and meaningful again.
What to Expect at Life Potential Chiropractic
Before we recommend any care plan, we start with a Stress Response Evaluation – a two-part assessment using Heart Rate Variability (HRV) analysis and brainwave analysis. This tells us how your nervous system is actually functioning – how much stress it’s holding, how well it’s adapting, and where the biggest imbalances are.
This matters because it helps us understand whether nervous system stress is amplifying your spinal stenosis symptoms, and how to design a care plan that addresses the root of what’s happening – not just the surface pain.
Care plans are typically 3-9 months, depending on how long the pattern has been present and what the assessment reveals. We check in regularly, re-evaluate, and adjust as the nervous system responds.
Combining Care Approaches
Network spinal care works well alongside other conservative treatments. If you’re working with a physical therapist or managing your stenosis with medication, that doesn’t disqualify you from this approach. In fact, addressing the nervous system can often make other interventions more effective – because when the body is less defended, it responds better to everything.
We’re also transparent about when surgery may genuinely be the right answer. If someone has severe stenosis with significant neurological deficits – loss of bowel or bladder control, rapid progression of weakness – those are situations where surgery should be on the table and we would say so directly. Most patients we see in Lancaster fall somewhere short of that threshold, and for them, conservative care is worth a real, committed effort before going under the knife.
Living with Spinal Stenosis in Lancaster
Spinal stenosis is one of those conditions that can quietly shrink your world. You stop walking as far. You avoid events that require a lot of standing. You plan your day around your pain. It’s not dramatic – it’s gradual – but over time it takes a real toll.
Many of the patients who come to Life Potential Chiropractic in Lancaster aren’t just looking for pain relief. They want their life back. They want to walk through Central Market without dreading the trip home. They want to keep up with their grandkids, or hike a trail, or just get through a workday without watching the clock.
That’s what we’re working toward with every patient – not just less pain, but better function, better adaptability, and a nervous system that’s working for you instead of against you.
Frequently Asked Questions
Q: Can spinal stenosis be treated without surgery?
A: For many people, yes. Conservative approaches including nervous system-focused care, physical therapy, and lifestyle modifications can significantly reduce symptoms and improve quality of life. Surgery is typically considered when conservative care has been given a real chance and symptoms continue to worsen, or when there are significant neurological deficits. We always assess each patient individually before making any recommendations.
Q: Is network spinal care safe for someone with spinal stenosis?
A: Network spinal uses very light, gentle touches – not forceful manipulation. It’s generally well-tolerated even by people with sensitive spinal conditions. That said, we conduct a thorough assessment before beginning care, and we tailor every care plan to what’s appropriate for your specific situation.
Q: How is this different from regular chiropractic adjustments?
A: Traditional chiropractic focuses primarily on moving vertebrae through manual manipulation – often involving that familiar popping or cracking sound. Network spinal care uses light, precise touches along the spine to work with the nervous system directly. There’s no forceful twisting or cracking involved, which makes it a different experience entirely – and often a better fit for people who are nervous about traditional adjustments or who have more complex spinal conditions.
If you’re dealing with spinal stenosis in Lancaster and want to explore your options, call us at (717) 847-6498 or book your $29 Discovery Session to get a real picture of what’s happening in your nervous system and what we can do about it.